The Journal of Respiratory Diseases
- The Journal of Respiratory Diseases Vol 6 No 12
- Volume 6
- Issue 12
Questions Physicians Often Ask About Allergens That Trigger Asthma
Abstract: Because of the impact of allergen exposure on asthma control, all patients with asthma should be evaluated for allergic sensitization. Such patients can be referred to an allergist for evaluation, or radioallergosorbent tests can be ordered by the primary care provider. The major groups of aeroallergens that can trigger asthma attacks include furred-pet, dust mite, cockroach, rodent, mold, and pollen allergens. When assessing a patient's exposure history, remember that furred-pet allergens are found not just in the home, but in other settings, such as schools, and these allergens are passively transferred from one environment to another. Allergen avoidance measures are essential to the management of asthma in sensitized patients and can significantly improve asthma control. First-line dust mite control measures include installing allergen-proof mattress and pillow encasements, washing all bedding every 1 to 2 weeks in hot water, removing stuffed toys, vacuuming and dusting regularly, and reducing indoor relative humidity. (J Respir Dis. 2006;27(12):511-526)
Allergic sensitization is an important risk factor for asthma, and allergen exposure in sensitized patients has been associated with increased asthma symptoms, greater medication requirements, and poorer lung function. In this article, we review the major allergens that can trigger asthma and describe the most effective avoidance measures.
THE KEY QUESTIONS
Why are allergens important in asthma?
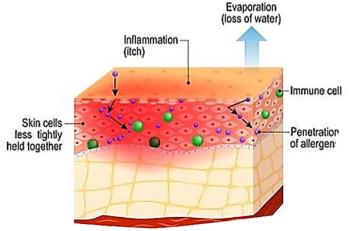
Allergen exposure is a known trigger of asthma, and the mechanism by which an allergen triggers respiratory symptoms is very well understood (Figure). A person must first become sensitized to an allergen to be at risk for the development of symptoms with subsequent exposure to the allergen.
Allergic sensitization is defined by the presence of allergen-specific IgE, and it occurs when a genetically susceptible person is exposed to an allergen. When the person becomes sensitized, the allergen- specific IgE binds to the surface of mast cells and basophils with no clinical consequence until reexposure occurs. On reexposure, the allergen binds to the cell surface- bound IgE, which triggers the mast cell to release histamine and other allergic mediators responsible for a cascade of inflammatory responses that result in symptoms.
Allergic sensitization is an important risk factor for asthma, particularly in children. About 80% of school-aged children with asthma have evidence of allergic sensitization to at least 1 common environmental allergen.1,2
Allergic sensitization to the predominant allergen in a community confers a 4- to 20-fold increase in the risk of asthma,3-5 suggesting a causal relationship between allergen exposure and the development of asthma. In sensitized patients with asthma, studies have clearly demonstrated that exposure can lead to both acute and chronic asthma symptoms.2,6-10
These findings have important implications for the clinical care of patients with asthma. Since allergen exposure plays an important role in triggering asthma symptoms, reducing allergen exposure is a logical component of treatment of the patient with allergic asthma. Reduction of exposure is feasible and risk-free, and it can result in improved asthma control.
Which patients should be evaluated for allergies?
To counsel patients and families appropriately regarding environmental control measures, one must know the specific allergic sensitizations of the patient. Therefore, all patients with asthma should be evaluated for allergic sensitization.
Patients can be referred to an allergist for evaluation, or radioallergosorbent tests (RASTs) can be ordered by the primary care provider. RASTs are performed by most commercial laboratories and are a measure of serum levels of allergen-specific IgE. Although RASTs are somewhat less sensitive than skin testing, they are helpful in determining whether a patient is likely to be allergic.11 For example, allergen exposure is very unlikely to be an important cause of asthma symptoms in a patient with negative results of RASTs using a panel of relevant allergens. However, a positive result of RAST to an allergen associated with a pet that is in the patient's home strongly suggests that pet exposure is a significant contributor to the patient's ongoing asthma symptoms and medication requirements.
What are the common allergens that trigger asthma?
Allergens are water-soluble glycoproteins, which induce an IgE response in susceptible persons. The allergens are adhered to particles that range in size from 1 µm to over 100 µm.12,13 Particles of this size are deposited into the upper and lower respiratory tracts, where the allergen can directly elicit an inflammatory response and subsequent respiratory symptoms.
Both indoor and outdoor allergens cause asthma symptoms. Indoor allergens are generally present year-round, so exposure to these allergens is associated with perennial symptoms. Outdoor allergens are generally present during circumscribed seasons and therefore trigger asthma symptoms during the relevant season.
Patients may have perennial allergen-induced asthma symptoms, seasonal allergen-induced symptoms, or both. For example, a patient presenting with persistent asthma with a history of springtime exacerbations may have asthma symptoms that are triggered by both perennial and seasonal allergens. There are 6 general groups of relevant aeroallergens: furred-pet, dust mite, cockroach, rodent, mold, and pollen allergens.
THE MAJOR AEROALLERGENS
Furred-pet allergens
Cats and dogs are common furred pets, although families often keep other species of furred pets as well. Cat and dog allergens can be found in virtually all homes, but homes with pets contain much higher levels of the allergens than do homes without pets.14 In addition, it is important to note that furred-pet allergens are also found in a variety of other settings, such as schools, and are passively transferred from one environment to another.8 Both cat and dog allergens are carried on small particles that remain airborne and adhere to surfaces and clothing.15-17
Allergic sensitization to these allergens is quite common, and in some populations more than 60% of children with asthma are sensitized to cat or dog allergens.18,19 However, the prevalence of sensitization varies depending on the composition of the predominant allergens in the community. The combination of widespread exposure and high prevalence of allergic sensitization indicates that a substantial proportion of persons with asthma are at risk for having cat or dog allergen-induced asthma symptoms. In fact, several studies have directly linked animal allergen exposure to poorer asthma outcomes among animal allergen-sensitized patients with asthma.8,20
Assessing pet allergen exposure in patients is fairly straightforward and can be accomplished by tak-ing a history focused on pet ownership; recent relocation into a home where pets had been living; and for children in particular, pet exposure at day care. Most relevant sources of exposure can be identified using this approach.
Because furred-pet allergens are airborne and adherent to clothing, it is impossible to eliminate exposure entirely. Pet removal is the only method of achieving substantial reductions in animal allergen levels, but allergen levels do not decline significantly for 4 to 6 months,21 so clinical benefit may not be realized for months. The rate of decline may be improved by vigorous cleaning to remove allergen remaining in reservoirs that include accumulated dust, carpeting, and bedding. Allergen-proof mattress and pillow encasings sequester the allergen in the mattress and pillow and are a helpful adjunct to pet removal (Table 1).
Because some families are very reluctant to give up a pet, alternative methods of furred-animal allergen control have been studied and have proved to be ineffective. Room high-efficiency particulate air (HEPA) filters can modestly reduce airborne animal allergens, but not to the degree necessary to improve asthma symptoms.22,23 Other methods, such as washing the pet, are also ineffective.24
Although the effect of pet removal on asthma symptoms has not been well studied because of the practical difficulties of conducting such an investigation, one recently published study demonstrated a substantial reduction in inhaled corticosteroid requirements among furred-pet allergen- sensitized adults with asthma who removed their pets from their homes, compared with those who kept their pets.25 These findings underscore that pet removal is a critical part of the treatment plan in pet allergen-sensitized patients with asthma.
Recent studies have suggested that exposure to pets early in life may protect against the development of allergies and asthma.26,27 However, it is not clear whether exposure to pets is directly responsible for protecting against asthma (see "Do pets protect against the development of asthma?").28
Dust mite allergens
Dust mites are arachnids that infest bedding, carpet, upholstered furniture, and fabric. Their main food source is human skin scales, and they grow best in warm, humid environments.29 As a result, they are rarely found in arid regions, such as the desert southwestern United States, but are common in the more humid regions. The predominant dust mites in the United States that have been implicated in allergic diseases are Dermatophagoides farinae and Dermatophagoides pteronyssinus.29,30 Dust mite allergens are predominantly found on larger particles, in the range of 10 to 20 µm, which rapidly settle on dependent surfaces after disturbance.13
The prevalence of allergic sensitization to house dust mites varies from region to region and depends on the regional prevalence of dust mites. For example, the sensitization rate among children with asthma has been estimated to be 5% in Los Alamos, New Mexico, in contrast to as high as 66% in Atlanta.5,31
Like many other allergens, exposure to dust mite allergen in sensitized patients has been associated with poorer lung function, great- er medication requirements, and more asthma symptoms.5,32,33 In contrast to other allergens, dust mite allergen has been identified as a causal agent in the pathogenesis of asthma. A prospective cohort study demonstrated that infants exposed to high levels of dust mite allergen were significantly more likely to have asthma later in childhood than were infants who were not exposed to high levels.3
In light of this evidence, the reduction of dust mite allergen exposure should both improve asthma control in sensitized patients and prevent the development of asthma in children.
Since dust mites are microscopic organisms, it is difficult to determine a patient's exposure status on the basis of history. The most practical approach is to assume that patients living in arid climates are very unlikely to have significant exposure to dust mites and that other patients in more humid regions are at risk for significant exposure.
First-line dust mite allergen control measures include installing allergen-proof mattress and pillow encasements, washing all bedding every 1 to 2 weeks in hot water, removing stuffed toys, vacuuming and dusting regularly, and reducing indoor relative humidity (Table 2). These strategies have been shown to reduce asthma symptoms, reduce medication requirements, and improve lung function.32-35
Removal of carpet and upholstered furniture may also be helpful, but it is more expensive. Because dust mite allergens are predominantly found on dependent surfaces and are not airborne, air filters are not likely to offer any benefit. Carpet treatments have also been developed and include agents that kill the dust mites (acaricides) as well as agents designed to denature the allergen. Although laboratory studies indicate that both of these reagents are effective, field studies indicate that neither are very effective.36,37
A recently published study found that mattress encasements as a single intervention provided no health benefit to adults with asth-ma.38 However, the patient population was unselected and therefore included patients who were not sensitized to dust mite allergen, as well as patients with other underlying lung disease, such as chronic obstructive pulmonary disease. This study provided little evidence to suggest that patients with asthma and dust mite allergen sensitization would not benefit from a multipronged dust mite intervention. In fact, the evidence accumulated thus far suggests that concerted efforts to control dust mite exposure are of clinical benefit in dust mite allergen-sensitized persons with asthma and are a critical component of the treatment plan for these patients.
Cockroach allergen
The 2 most common cockroaches found in homes in the United States are the German cockroach (Blatella germanica) and the American cockroach (Periplaneta americana). Most sensitized persons appear to be primarily sensitized to German cockroach allergen, which has been studied extensively.
Cockroach allergen is the predominant allergen in the inner city, where most homes contain detectable levels.2 At least half of inner-city homes have clinically relevant levels of cockroach allergen. Although as many as 30% of suburban middle-class homes also contain detectable levels of cockroach allergen, the levels in suburban homes are much lower than levels found in inner-city homes.39,40
In inner-city populations, 30% to 40% of children with asthma are sensitized to cockroach allergen,41 and in suburban populations, sensitization rates are about 21%.39 Cockroach allergen has also been directly linked to poorer asthma outcomes in inner-city children with asthma, including asthma- related health care use.2
In light of these findings, it is important to assess the risk of exposure in sensitized patients and make recommendations for reducing cockroach allergen exposure (Table 3). Although patient report of cockroach infestation is a good indicator of significant levels of cockroach allergen exposure,40 one cannot be reassured that a patient who denies cockroach infestation is not being exposed to significant levels of the allergen. Patients may be reluctant to admit pest infestation, and homes without evidence of active infestation often contain substantial levels of the allergen.
Cockroach allergen levels can be substantially reduced by using an integrated pest management approach. Several studies have demonstrated that a combination of extermination, vigorous cleaning aimed at reducing reservoir allergen, and meticulous care in disposing of food remains can result in 80% to 90% reductions in cockroach allergen levels.42,43
It remains unknown whether this degree of allergen reduction will have a clinical impact. However, the strong evidence that cockroach allergen exposure is linked with asthma morbidity supports recommending an integrated pest management approach to reduce exposure in cockroach allergen- sensitized patients with asthma.
Rodent allergens
Mice and rats excrete urinary allergens that are carried on small particles that readily become airborne.44-47 The allergens are pheromone-binding proteins that are thought to have a role in mating practices48 and are excreted in very large quantities in the urine. Although these allergens have long been known to cause occupational asthma, their role in nonoccupational asthma has only recently been described.9,49
The domestic house mouse is very common, particularly in urban areas where multifamily dwellings and poorly maintained housing are common.50 Mouse allergen can be found in virtually all inner-city homes, and one study found detectable airborne mouse allergen in 84% of bedrooms of inner-city children with asthma.51 Mouse allergen levels in some homes are similar to levels measured in occupational settings, where mouse allergen is a known cause of asthma symptoms.
Mouse allergen is surprisingly prevalent in suburban communities as well, with as many as 75% of suburban middle-class households having detectable mouse allergen levels in settled dust samples.52,53 However, it is important to note that the levels in these suburban homes are 100- to 1000-fold lower than the levels observed in inner-city settings. Recent studies have linked exposure to mouse allergen to poorer asthma control and an increased risk of asthma-related health care use among mouse allergen-sensitized inner-city children with asthma.7,9
Assessing exposure to mouse allergen can be fairly straightforward. Any patient who reports mouse sightings or evidence of mice, such as droppings, is very likely to be exposed to significant levels of mouse allergen in the home.50-52 However, as with cockroach allergen, patients and families may be reluctant to admit a rodent infestation, so a negative history is not a good predictor of lack of exposure. In addition, substantial levels of mouse allergen can be found in homes with little or no evidence of infestation, because mice nest in hidden spaces and are active at night.
Reducing exposure to mouse allergen is feasible, but it can be difficult. Integrated pest management is the best approach and includes a combination of extermination; vigorous cleaning; meticulous disposal of food remains; and sealing of holes and cracks in walls, doors, and ceilings (Table 4). Using this approach, the allergen source is eliminated, the allergen reservoirs are cleaned up, and reinfestation is discouraged.
In one study, integrated pest management resulted in a 75% reduction in mouse allergen levels in settled dust, while levels increased in the control group.54 Although no studies have been conducted to determine the impact of mouse allergen reduction on asthma, the evidence to date indicates that reduction of exposure will improve asthma control and prevent asthma-related morbidity.
Rats are also common in urban areas, and although they typically do not venture indoors, rat allergen has been found in 33% of inner-city homes. In one multicenter study, 21% of inner-city children with asthma were sensitized to rat allergen, and the children who were sensitized and exposed to rat allergen in their homes were at greater risk for asthma-related hospitalization and unscheduled medical visits than children who were not sensitized or exposed.10 No published studies have examined methods of reducing household rat allergen, but a reasonable approach would include sealing holes and cracks in the home's structure, vigorous cleaning to remove reservoir allergen, and extermination.
Pollen allergens
Tree, grass, and weed pollens are present in all regions of the United States and are known to cause seasonal exacerbations of asthma. Tree pollen is produced primarily in the spring, with levels peaking at slightly different times depending on the regional climate. Grass pollen levels peak in the summer, and weed pollen levels peak in the fall. Again, the peak of these seasons varies by region, so an understanding of the timing of pollen seasons in one's region is quite helpful when evaluating a patient who has a history of seasonal asthma exacerbations.
Pollen allergen sensitization is common. For example, a population-based study found that more than 25% of the US population is sensitized to ragweed allergen, and a similar proportion of the population is sensitized to grass pollen allergen.55 The well-known phenomenon of pollen-induced asthma is characterized by a predictable increase in asthma symptoms during the relevant pollen season in a sensitized patient.
Unfortunately, it is very difficult to reduce pollen allergen exposure during the pollen season. Recommendations for exposure reduction include staying indoors, keeping windows and doors closed, using air conditioning, and perhaps using room HEPA filters. After spending time outdoors, pollen-allergic patients should wash their hands and face and wash their hair daily to remove the allergen.
Mold allergens
There is a very large number of mold species, and very few have been well studied for their effects on asthma. Molds can be found in both indoor and outdoor environments. Aspergillus and Penicillium species are among the most common indoor molds, and Alternaria can be found in both indoor and outdoor environments.
Molds have been extremely difficult to study because of their complexity. However, major allergens have been isolated from a few molds, and sensitization to Alternaria has been linked to the development of asthma, as well as to asthma severity in midwestern and southwestern US populations.56,57 It is important to note, however, that Alternaria is found in all regions of the country.58
Because molds prefer warm, moist environments, mold growth can be prevented by interventions aimed at reducing moisture and humidity (Table 5). These interventions should include dehumidification, air conditioning, and increased ventilation. Some families use humidifiers or vaporizers, which can contribute to indoor humidity and become colonized with mold, so these items should be banned. For mold that is already present, thorough cleaning with fungicides is recommended, and when cleaning is not possible, the item should be discarded.
Keeping windows closed and running the air conditioner may help reduce exposure to outdoor sources of mold. A room HEPA filter may also help, but the effectiveness of this intervention has not been studied. When outdoors, patients should avoid heavy exposure to moldy vegetation and use a properly fitting particulate mask when working with moldy material. Although there have been no randomized trials of the effectiveness of mold abatement in persons with asthma, there is adequate evidence to recommend these basic interventions to reduce exposure for mold allergen-sensitized patients with asthma.
References:
REFERENCES
1. Huss K, Adkinson NF Jr, Eggleston PA, et al. House dust mite and cockroach exposure are strong risk factors for positive allergy skin test responses in the Childhood Asthma Management Program.
J Allergy Clin Immunol
. 2001;107:48-54.
2. Rosenstreich DL, Eggleston P, Kattan M, et al. The role of cockroach allergy and exposure to cockroach allergen in causing morbidity among inner-city children with asthma.
N Engl J Med
. 1997;336:1356-1363.
3. Sporik R, Holgate ST, Platts-Mills TA, Cogswell JJ. Exposure to house-dust mite allergen (Der p I) and the development of asthma in childhood. A prospective study.
N Engl J Med
. 1990;323:502-507.
4. Squillace SP, Sporik RB, Rakes G, et al. Sensitization to dust mites as a dominant risk factor for asthma among adolescents living in central Virginia. Multiple regression analysis of a population-based study.
Am J Respir Crit Care Med
. 1997;156:1760-1764.
5. Call RS, Smith TF, Morris E, et al. Risk factors for asthma in inner city children.
J Pediatr
. 1992;121:862-866.
6. Litonjua AA, Carey VJ, Burge HA, et al. Exposure to cockroach allergen in the home is associated with incident doctor-diagnosed asthma and recurrent wheezing.
J Allergy Clin Immunol
. 2001;107:41-47.
7. Phipatanakul W, Celedon JC, Sredl DL, et al. Mouse exposure and wheeze in the first year of life.
Ann Allergy Asthma Immunol
. 2005;94:593-599.
8. Almqvist C, Wickman M, Perfetti L, et al. Worsening of asthma in children allergic to cats, after indirect exposure to cat at school.
Am J Respir Crit Care Med
. 2001;163:694-698.
9. Matsui EC, Eggleston PA, Buckley TJ, et al. Household mouse allergen exposure and asthma morbidity in inner-city pre-school children.
Ann Allergy Asthma Immunol
. In press.
10. Perry T, Matsui E, Merriman B, et al. The prevalence of rat allergen in inner-city homes and its relationship to sensitization and asthma morbidity.
J Allergy Clin Immunol
. 2003;112:346-352.
11. Yunginger JW, Ahlstedt S, Eggleston PA, et al. Quantitative IgE antibody assays in allergic diseases.
J Allergy Clin Immunol
. 2000; 105:1077-1184.
12. Wood RA, Laheri AN, Eggleston PA. The aerodynamic characteristics of cat allergen.
Clin Exp Allergy
. 1993;23:733-739.
13. Platts-Mills TA, Heymann PW, Longbottom JL, Wilkins SR. Airborne allergens associated with asthma: particle sizes carrying dust mite and rat allergens measured with a cascade impactor.
J Allergy Clin Immunol
. 1986;77:850-857.
14. Bollinger ME, Eggleston PA, Flanagan E, Wood RA. Cat antigen in homes with and without cats may induce allergic symptoms.
J Allergy Clin Immunol
. 1996;97:907-914.
15. Wood RA, Mudd KE, Eggleston PA. The distribution of cat and dust mite allergens on wall surfaces.
J Allergy Clin Immunol
. 1992;89:126-130.
16. Custovic A, Simpson B, Simpson A, et al. Relationship between mite, cat, and dog allergens in reservoir dust and ambient air.
Allergy
. 1999;54: 612-616.
17. Munir AK, Einarsson R, Dreborg S. Variability of airborne cat allergen, Fel d1, in a public place.
Indoor Air
. 2003;13:353-358.
18. Munir AK, Bjorksten B, Einarsson R, et al. Cat (Fel d I), dog (Can f I), and cockroach allergens in homes of asthmatic children from three climatic zones in Sweden.
Allergy
. 1994;49:508-516.
19. Sporik R, Ingram JM, Price W, et al. Association of asthma with serum IgE and skin test reactivity to allergens among children living at high altitude. Tickling the dragon's breath.
Am J Respir Crit Care Med
. 1995;151:1388-1392.
20. Lewis SA, Weiss ST, Platts-Mills TA, et al. The role of indoor allergen sensitization and exposure in causing morbidity in women with asthma.
Am J Respir Crit Care Med
. 2002;165:961-966.
21. Wood RA, Chapman MD, Adkinson NF Jr, Eggleston PA. The effect of cat removal on allergen content in household-dust samples.
J Allergy Clin Immunol
. 1989;83:730-734.
22. Wood RA, Johnson EF, Van Natta ML, et al. A placebo-controlled trial of a HEPA air cleaner in the treatment of cat allergy.
Am J Respir Crit Care Med
. 1998;158:115-120.
23. Gore RB, Bishop S, Durrell B, et al. Air filtration units in homes with cats: can they reduce personal exposure to cat allergen?
Clin Exp Allergy
. 2003; 33:765-769.
24. Nageotte C, Park M, Havstad S, et al. Duration of airborne Fel d 1 reduction after cat washing.
J Allergy Clin Immunol
. 2006;118:521-522.
25. Shirai T, Matsui T, Suzuki K, Chida K. Effect of pet removal on pet allergic asthma.
Chest
. 2005; 127:1565-1571.
26. Ownby DR, Johnson CC, Peterson EL. Exposure to dogs and cats in the first year of life and risk of allergic sensitization at 6 to 7 years of age.
JAMA
. 2002;288:963-972.
27. Platts-Mills T, Vaughan J, Squillace S, et al. Sensitisation, asthma, and a modified Th2 response in children exposed to cat allergen: a population-based cross-sectional study.
Lancet
. 2001;357:752-756.
28. Ownby DR, Johnson CC. Does exposure to dogs and cats in the first year of life influence the development of allergic sensitization?
Curr Opin Allergy Clin Immunol
. 2003;3:517-522.
29. Arlian LG. Dust mites: update on their allergens and control.
Curr Allergy Asthma Rep
. 2001; 1:581-586.
30. Platts-Mills TA, Thomas WR, Aalberse RC, et al. Dust mite allergens and asthma: report of a second international workshop.
J Allergy Clin Immunol
. 1992;89:1046-1060.
31. Ingram JM, Sporik R, Rose G, et al. Quantitative assessment of exposure to dog (Can f 1) and cat (Fel d 1) allergens: relation to sensitization and asthma among children living in Los Alamos, New Mexico.
J Allergy Clin Immunol
. 1995;96:449-456.
32. Ehnert B, Lau-Schadendorf S, Weber A, et al. Reducing domestic exposure to dust mite allergen reduces bronchial hyperreactivity in sensitive children with asthma.
J Allergy Clin Immunol
. 1992; 90:135-138.
33. Custovic A, Taggart SC, Francis HC, et al. Exposure to house dust mite allergens and the clinical activity of asthma.
J Allergy Clin Immunol
. 1996;98:64-72.
34. Carswell F, Birmingham K, Oliver J, et al. The respiratory effects of reduction of mite allergen in the bedrooms of asthmatic children--a double-blind controlled trial.
Clin Exp Allergy
. 1996;26: 386-396.
35. Halken S, Host A, Niklassen U, et al. Effect of mattress and pillow encasings on children with asthma and house dust mite allergy.
J Allergy Clin Immunol
. 2003;111:169-176.
36. Woodfolk JA, Hayden ML, Couture N, Platts-Mills TA. Chemical treatment of carpets to reduce allergen: comparison of the effects of tannic acid and other treatments on proteins derived from dust mites and cats.
J Allergy Clin Immunol
. 1995; 96:325-333.
37. Hayden ML, Rose G, Diduch KB, et al. Benzyl benzoate moist powder: investigation of acaricidal [correction of acarical] activity in cultures and reduction of dust mite allergens in carpets.
J Allergy Clin Immunol
. 1992;89:536-545.
38. Woodcock A, Forster L, Matthews E, et al. Control of exposure to mite allergen and allergen-impermeable bed covers for adults with asthma.
N Engl J Med
. 2003;349:225-236.
39. Matsui EC, Wood RA, Rand C, et al. Cockroach allergen exposure and sensitization in suburban middle-class children with asthma.
J Allergy Clin Immunol
. 2003;112:87-92.
40. Cohn RD, Arbes SJ Jr, Jaramillo R, et al. National prevalence and exposure risk for cockroach allergen in U.S. households.
Environ Health Perspect
. 2006;114:522-526.
41. Eggleston PA, Rosenstreich D, Lynn H, et al. Relationship of indoor allergen exposure to skin test sensitivity in inner-city children with asthma.
J Allergy Clin Immunol
. 1998;102:563-70.
42. Eggleston PA, Wood RA, Rand C, et al. Removal of cockroach allergen from inner-city homes.
J Allergy Clin Immunol
. 1999;104:842-846.
43. Arbes SJ Jr, Sever M, Mehta J, et al. Abatement of cockroach allergens (Bla g 1 and Bla g 2) in low-income, urban housing: month 12 continuation results.
J Allergy Clin Immunol
. 2004;113: 109-114.
44. Schumacher MJ, Tait BD, Holmes MC. Allergy to murine antigens in a biological research institute.
J Allergy Clin Immunol
. 1981;68:310-318.
45. Platts-Mills TA, Longbottom J, Edwards J, et al. Occupational asthma and rhinitis related to laboratory rats: serum IgG and IgE antibodies to the rat urinary allergen.
J Allergy Clin Immunol
. 1987; 79:505-515.
46. Ohman JL Jr, Hagberg K, MacDonald MR, et al. Distribution of airborne mouse allergen in a major mouse breeding facility.
J Allergy Clin Immunol
. 1994;94:810-817.
47. Eggleston PA, Ansari AA, Ziemann B, et al. Occupational challenge studies with laboratory workers allergic to rats.
J Allergy Clin Immunol.
1990;86:63-72.
48. Sharrow SD, Vaughn JL, Zidek L, et al. Pheromone binding by polymorphic mouse major urinary proteins.
Protein Sci
. 2002;11:2247-2256.
49. Phipatanakul W, Eggleston PA, Wright EC, Wood RA; National Cooperative Inner-City Asthma Study. Mouse allergen. II. The relationship of mouse allergen exposure to mouse sensitization and asthma morbidity in inner-city children with asthma.
J Allergy Clin Immunol
. 2000;106: 1075-1080.
50. Chew GL, Perzanowski MS, Miller RL, et al. Distribution and determinants of mouse allergen exposure in low-income New York City apartments.
Environ Health Perspect
. 2003;111:1348-1351.
51. Matsui EC, Simons E, Rand C, et al. Airborne mouse allergen in the homes of inner-city children with asthma.
J Allergy Clin Immunol
. 2005;115: 358-363.
52. Matsui EC, Wood RA, Rand C, et al. Mouse allergen exposure and mouse skin test sensitivity in suburban, middle-class children with asthma.
J Allergy Clin Immunol
. 2004;113:910-915.
53. Cohn RD, Arbes SJ Jr, Yin M, et al. National prevalence and exposure risk for mouse allergen in US households.
J Allergy Clin Immunol
. 2004; 113:1167-1171.
54. Phipatanakul W, Cronin B, Wood RA, et al. Effect of environmental intervention on mouse allergen levels in homes of inner-city Boston children with asthma.
Ann Allergy Asthma Immunol
. 2004; 92:420-425.
55. Arbes SJ Jr, Gergen PJ, Elliott L, Zeldin DC. Prevalences of positive skin test responses to 10 common allergens in the US population: results from the third National Health and Nutrition Examination Survey.
J Allergy Clin Immunol
. 2005;116: 377-383.
56. Bush RK, Prochnau JJ.
Alternaria
-induced asthma.
J Allergy Clin Immunol
. 2004;113:227-234.
57. Halonen M, Stern DA, Wright AL, et al.
Alternaria
as a major allergen for asthma in children raised in a desert environment.
Am J Respir Crit Care Med
. 1997;155:1356-1361.
58. Salo PM, Yin M, Arbes SJ Jr, et al. Dustborne
Alternaria alternata
antigens in US homes: results from the National Survey of Lead and Allergens in Housing.
J Allergy Clin Immunol
. 2005;116:623-629.
Articles in this issue
about 19 years ago
Diagnostic Puzzlers: A patient with an "extra" pulmonary blood vesselabout 19 years ago
Clinical Consultation: Noninvasive ventilation for COPDNewsletter
Enhance your clinical practice with the Patient Care newsletter, offering the latest evidence-based guidelines, diagnostic insights, and treatment strategies for primary care physicians.